 Intervention of the Month Intervention of the Month |
|
| A Myocardial Abscess Presented as Acute Myocardial Infarction |
Won Yu Kang, MD, Jong Chun Park, MD, PhD, Hyun Ju Yoon, MD, Ju Han Kim, MD, PhD and Myung Ho Jeong, MD, FACC, FAHA, FESC, FSCAI
The Heart center of Chonnam National University Hospital, Gwangju, Korea
|
|
A 46-year-old woman had suffered from left anterior chest pain lasting 2 days visited our hospital. She had been undergoing chemotherapy for 3 years due to myelodysplastic syndrome. She did not ever smoke and does not have medical history of diabetes or hypertension. Her blood pressure on admission was 120/80 mmHg and body temperature was 36.5 ℃.
Her electrocardiogram (ECG) at admission showed ST segment elevation in V2-V4 with T wave inversion in V2-V5 (Fig. 1). In initial laboratory examination, bicytopenia was detected (WBC count = 1,300 /mm3, platelet count = 5,000 /mm3). Her cardiac markers were within normal limit (Troponin I = 0.001 ng/mL, CK-MB = 5.1 U/L, AST = 14 U/L) and C-reactive protein was elevated up to 21.5 mg/dL (reference level= 0~0.3 mg/dL). Transthoracic echocardiogram performed with suspicion of acute coronary syndrome revealed hypokinesia in apical septal and apical anterior wall of left ventricle (LV). In apical pericardial area just adjacent hypokinetic lesion, hypoechoic lesion was found, it suggested abscess (TTE, Fig. 2). The size of lesion was 27.2 x 11.9 mm in the 2D echocardiogram. Cardiac computed tomography demonstrated mild diffuse thickening with contrast enhancement of pericardium and loculated fluid collection in anterior myocardium and pericardium without definite luminal narrowing in coronary arteries (Fig. 3).
We consulted to thoracic surgeon and interventional radiologist for tissue diagnosis. But her extremely lower platelet count and small size of the lesion made them to hesitate to do invasive diagnostic procedure. We had to give her conservative treatment with antibiotics (third generation cephalosporin plus aminoglycoside). Follow-up TTE had done in 2 weeks later since the first exam showed no significant interval changes (Fig. 4-A and B). Follow-up chest CT conducted 3 weeks later since antibiotics treatment revealed marked improvement of previous seen loculated fluid collection in anterior myocardiaum and pericardium, but still remained focal wall thickening and enhancement (Fig. 5). Follow-up 2D echocardiogram done in 7 weeks later demonstrated complete resolution of the lesion (Fig. 4-C and D).
Myocardial abscess, a suppurative infection of the myocardium, endocardium, valves, perivalvular structures, or the cardiac conduction system, have been described very rarely.1 Generally, this disease occurs as a complication of infective endocarditis, acute myocardial infarction, or other infections in the setting of debilitating condition. In our case, interestingly, there was no definite infection focus or coronary obstruction in cardiac CT. To the best of our knowledge, this is the first report concerning the possibility of occurrence of myocardial abscess presented as AMI, not a following consequence of AMI.
|
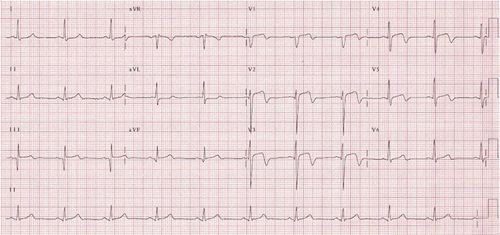 |
▲ Figure 1. Electrocardiogram at admission, showing ST segment elevation in V2-V4 and T wave inversion in V2-V5.
|
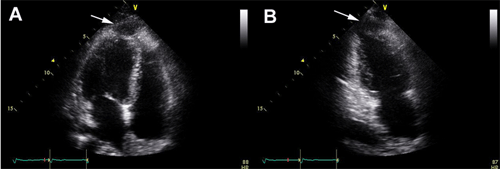 |
▲ Figure 2. 2D Echocardiogram. (A) Apical 4 chamber view shows hypokinesia in apical septal wall of left ventricle ( LV ) and hypoechoic lesion (arrow) in apical pericardial area just adjacent hypokinetic lesion. (B) Apical 2 chamber view reveals hypokinesia in apical anterior wall of LV and hypoechoic lesion (arrow) in pericardial area. Note that the maximal size was 27.2 x 11.9 mm.
|
 |
▲ Figure 3. Cardiac computed tomography (CT). (A) Volume rendering image shows no critical narrowing in either coronary arteries. (B, C, and D) Cardiac CT demonstrates mild diffuse thickening with contrast enhancement of pericardium and loculated fluid collection in apical anterior pericardium (arrows). Note that left anterior descending coronary artery runs beside by the lesion (arrowhead in panel B).
|
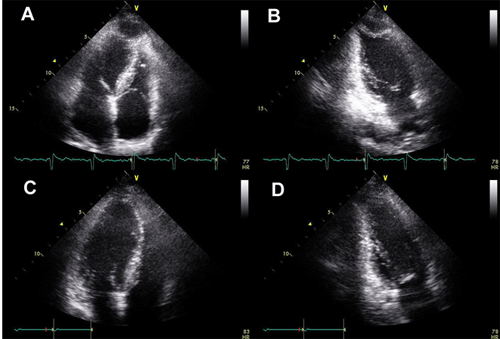 |
▲ Figure 4. Follow-up 2D Echocardiogram. (A and B) 2D Echocardiogram performed 2 weeks later shows no significant interval change of pericardial hypoechoic lesion in size. (C and D) 2D echocardiogram carried out 7 weeks later demonstrates complete resolution of the lesion.
|
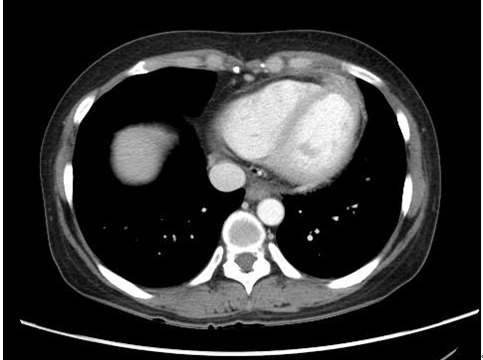 |
▲ Figure 5. Follow-up chest computed tomography after 3 weeks of antibiotics treatment, showing marked improvement of previous seen loculated fluid collection in anterior pericardium, but still remained focal wall thickening and enhancement.
|
|
| |
위의 이달의 중재술을 보신 선생님들의 의견을 아래의 의견 쓰기에 의견을 남겨 주십시오.
선생님들의 다양한 의견을 받습니다.
|
![[의견쓰기]](/image/comment_btn.gif) |
Warning: include(/home/virtual/circulationadmin/new/info/comment_index.php) [function.include]: failed to open stream: No such file or directory in /home/virtual/circulationadmin/new/info/case/200811/case200811.htm on line 176
Warning: include() [function.include]: Failed opening '/home/virtual/circulationadmin/new/info/comment_index.php' for inclusion (include_path='.:/usr/local/php/lib/php') in /home/virtual/circulationadmin/new/info/case/200811/case200811.htm on line 176
|
|
|